Pressure Sores
Pressure ulcers, also known as decubitus ulcers or bedsores, are lesions caused by unrelieved pressure on soft tissues overlying a bony prominence which reduces or completely obstructs the blood flow to the superficial tissues. Most commonly this will be the sacrum or the hips, but other sites such as the elbows, knees, ankles or the back of the cranium can be affected. It is widely believed that other factors can influence the occurrence and development of pressure ulcers. Among these are friction and shearing forces applied to the affected skin when the person is moved, humidity caused by sweating or incontinence, the age of the person which may reflect their healing ability, other ongoing medical conditions (such as diabetes or infection) or medication which may affect the person's cardio-circulatory system or their ability to move easily in bed or in a wheelchair. Although often prevented and treatable if found early, they can be very difficult to prevent in frail elderly patients, wheelchair users (especially where spinal injury is involved) and terminally ill patients. Bedsores are often fatal—even under the auspices of medical care—and are one of the leading iatrogenic causes of death reported in developed countries, second only to adverse drug reactions. The primary cure and treatment is to remove the pressure by turning the patient regularly (every two hours is often quoted, though the evidence for this figure is not strong and every four hours may be just as effective with some patients). However the relief of pressure to avoid further sores is well documented since at least the 19th century; regular turning was advised to prevent sores by Galloway.
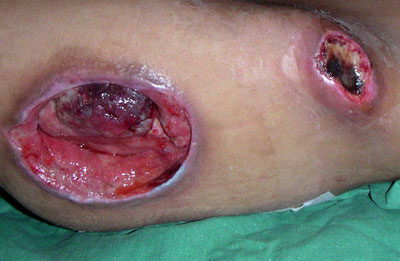
Preventive care
The most important care for a patient with bedsores is the relief of pressure. Once a bedsore is found, pressure should immediately be lifted from the area and the patient turned at least every two hours to avoid aggravating the wound. Nursing homes and hospitals usually set programs to avoid the development of bedsores in bedridden patients such as using a standing frame to reduce pressure and ensuring dry sheets by using catheters or impermeable dressings. For individuals with paralysis, pressure shifting on a regular basis and using a cushion featuring pressure relief components can help prevent pressure wounds.
Pressure-distributive mattresses are used to reduce high values of pressure on prominent or bony areas of the body.[ Antidecubitus mattresses and cushions can contain multiple air chambers that are alternately pumped. However, methods to evaluate the efficacy of these products have only been developed in recent years.

Casaflex Pressure Relieving Mattress
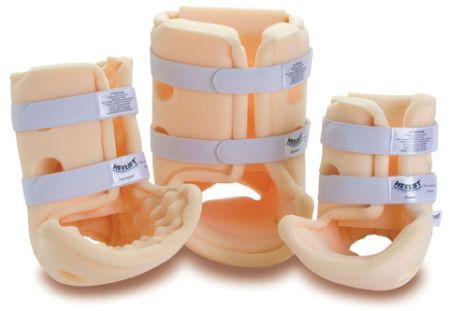
Ankle / Heel Pressure Relief Support






